What’s Causing the Home Health Aide Staffing Shortage?
I thought it would make sense to write about the state of affairs regarding home health aide staffing.
Staffing shortages are affecting nearly every industry, including health care. We are currently seeing shortages in retail stores like Walmart and Target because our supply chain is suffering from a lack of workers at nearly every step of the supply chain. Dockworkers, port workers, truck drivers, and retail personnel are all in high demand and low supply.
The healthcare industry is no different. Keep reading to learn how this issue developed and how you can navigate in-home senior care in the future.
The Decline in Home Health Aide Job Enrollment
Back in 2019, before COVID existed, our industry was experiencing an employment crisis. Home health aides, nurse’s aides, and nurses were all in the top 10 most in-demand jobs nationwide in 2019.
In 2016, the most in-demand jobs in the healthcare field were direct care workers. This category included Personal Care Aide, Home Health Aide, and Certified Nursing Assistant positions. So this is nothing new. We have never had enough direct care and frontline workers over the last decade, but COVID has exacerbated this problem.
When things were going well, we needed aides and nurses. Now with COVID and the future being uncertain at best, we are feeling the crunch even more. We are seeing a lack of nurses, both RN and LPNs, and a lack of CNAs and HHAs, our main caregivers who provide care for people at home, on hospice, in assisted living, and skilled nursing homes (both long-term and short-term).
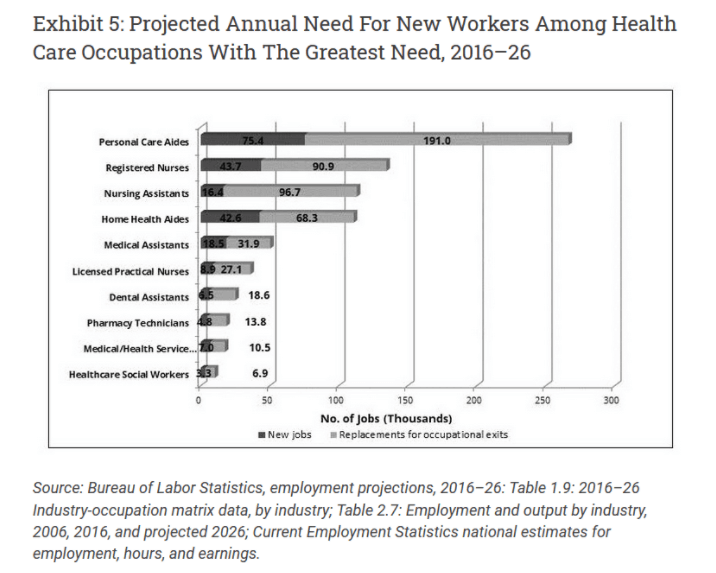
As you can see below, this chart shows the projected need for new workers in the healthcare industry. It is no surprise that home health aides and nurses make up the top four in-demand occupations.
In other words, most home care agencies are all pulling caregivers from the same shrinking pool of applicants.
Are you looking for caregivers with the best training?
Why Is the Home Health Aide Employment Pool So Much Smaller?
What has caused the employment pool to become tighter? A few areas are big reasons why people cannot find caregivers to hire in the Boston area.
COVID-19
Let’s get the obvious factor out of the way. COVID-19 has caused many people, including caregivers, to reconsider what they want from their careers. Caring for the elderly is a job mainly held by African immigrants who are sending remittances back home. But many of these caregivers have found it too dangerous to work on the front lines and risk contracting an infectious disease.
Additionally, wearing PPE every day for over a year has been another friction point caused by COVID. People are sick and tired of COVID, and wearing PPE every day has overstayed its welcome. With other opportunities available, frontline workers are considering other options.
Immigration
Immigration has also caused fewer caregivers to come to the United States. With COVID, we have seen bans on visas and immigration, which has left many jobs open that were popular with immigrants looking for work.
COVID has caused long delays in getting the proper documentation to come to the United States, putting a squeeze on many industries that offer jobs to immigrants looking for a better life. The administrative red-tape that is already complicated and cumbersome has seen wait times increase as policies have changed how quickly employers can process applications.
Additionally, reports are that the current administration is putting bans on all visas from individuals who have not received a vaccination, which is the vast majority of the world, especially in countries like Africa.
“This move, which is effectively a ban on Africa, is wrong, and he should reconsider. The economic costs will be significant. Nearly half a million people travel to the United States from Africa during normal years. In addition, nearly 60,000 permanent immigrants settle here. This ban will harm the United States.”
That’s many people who normally would come to the US to work. With fewer immigrants coming into the country, the supply is smaller and the demand greater on finding service and manual labor workers.
Child Care
Child care has also been a hurdle to overcome. Before the pandemic, kids were in schools, families had sitters, and neighbors could watch kids.
Once COVID came, all of that ended. Schools closed, and learning occurred at home, supervised by a parent who no longer could work as a caregiver.
Neighbors and sitters were in the same situation. Because of the uncertainty and dangers of COVID, no one trusted people to come into their homes unless necessary. This fear again limited the number of caregivers who could accept jobs caring for the elderly.
Parents who are caregivers found themselves choosing between work and remote learning childcare. It’s not a difficult decision to make. Family care will always come before work.
State and Federal Benefits
Government benefits eased the financial burden of leaving your job due to COVID. When caregivers realized they would make nearly as much, if not more, through state unemployment plus the $300/week federal benefit, caregivers (as well as many other lower-paid workers) did some basic math and left their jobs.
Many of these caregivers then looked for untaxed “under-the-table” positions with families to supplement their income during the hours they could work, double-dipping and increasing their take-home each month.
Families have seen additional benefits for having children. The idea is that paying them direct cash benefits will allow them to afford child care. In turn, this stipend will free them to go back to work.
The overall point is that benefits have incentivized caregivers to stay at home rather than go back to work. I don’t blame them. Why would I say no if you offered me the same pay or higher to stay home?
This choice certainly is an indictment of the wages that caregivers in the USA receive. These wages will likely increase further because of COVID and the low supply with high demand for caregivers.
Supply and Demand
For most of our employees, working with seniors is a passion. Caring for others is part of their DNA, but it is not the only factor in where they work, as many are supporting loved ones back in Africa. With so many retail, warehouse, and other manual labor jobs available, caregivers have opened up new opportunities to change fields and go into other industries.
With immigration limited and so many frontlines, customer-facing positions open, it has increased the demand for all workers, increasing the cost of employing individuals. The more caregivers get paid, the more customers need to be charged, which is why we see unprecedented increases in home care and nursing home rates.
Realize that a caregiver’s salary has a direct correlation to what the customer pays. When corporations experience increased costs that can not be eliminated or offset, they pass that cost increase onto the customer. That’s why inflation is a trending topic these days.
The Limitations of Low-Hour Cases for Home Health Aides
The above factors placed limitations on what home care, nursing home, and assisted living providers can accomplish. There are not enough home health aide applicants for everyone, causing agencies to miss their required staff-to-resident ratios. Home care companies have no choice but to decline short-hour cases as it is impossible to staff them.
We are getting calls from families looking for eight, twelve, or twenty hours a week of care. Many of these customers have had no luck with the dozen other caregiver agencies they have called. At this point, there is no point in accepting these cases. Even if we can staff the case, it will only be for a few shifts before the caregiver has accepted a new case with us or a competing home care agency. There is no point providing hope to the family, only to let them down a week later and tarnish our reputation. It is better to decline the case and let them keep searching.
Key Takeaways
How long this will last is anyone’s guess. With the Delta variant surging into fall and winter, I do not see the home health aide shortage changing anytime soon. The rate will likely continue to increase in hopes of attracting caregivers.
The downside of this is that it prices more families out of the market. As prices increase throughout the senior care industry, fewer families can afford the minimum needed care. This domino effect places more strain on family caregivers. Ultimately, this trend has a ripple effect on work, the community, an individual’s retirement, and the economy as a whole.
If you have questions about our private home care services, get in touch with us here!